Innovations in healthcare provide us with better care. In the past innovations like MRI have shocked the world. In 1946 a study in the field of physics observed how normal matter interacted with magnetic waves. Based on these advances MRI was invented in 1977 and it dramatically changed the world by becoming a critical tool for getting a complete picture of the patient’s body. MRI makes it easier for healthcare professionals to make a diagnosis of a disease.
Innovations in Artificial Intelligence (AI) are already present in our world in several ways, especially when using the internet. AI is used for almost everything from online shopping to searching. However, in public institutions like healthcare the use of AI innovations is less prominent and in the Netherlands merely 5% of clinicians use AI applications. While healthcare uses and creates a lot of data on which some form of AI can be applied, we believe it is not used to its full potential. In certain areas such as pattern recognition which can be a tedious process for doctors, doctors can be replaced by AI applications. In other areas such as classification, innovations are developed that could save clinicians time. Combined with the overwork and shortage of time doctors cope with, AI in healthcare might be the solution.
Furthermore, AI used for the prevention, diagnosis and treatment of obesity, dementia and breast cancer alone could yield cost savings of over 170 billion. Since the vast rise of healthcare spending, due to aging, is forming a significant problem in most western countries, cost savings with AI in healthcare need to be done. Because of this we argue that healthcare is currently lagging behind in terms of AI
AI innovations currently used
Currently, several AI innovations have been implemented in healthcare. The most important innovations are listed below and are divided under different sections. These sections represent the key techniques within AI: Machine Learning (ML), Natural Language Processing (NLP) and robots. Of course, not all innovations are mentioned, but the main ones are listed to create a global overview.
Machine Learning
ML is the concept of teaching a computer to think like a human which then allows it to keep on learning from all the data it captures. Using ML, patterns can be recognized. With these patterns, ML algorithms are able to make predictions. By training an ML algorithm, it is able to learn continue its learning process, which makes its predictions more accurate.
A first way to use ML in health care is by Decision Support Systems (DSS). In The Netherlands, a DSS has already been implemented to support the decision between photon or proton therapy for patients suffering from neck or head cancer. The DSS is successfully being used and is very cost efficient. Another field where DSSs are currently used is neurosurgery. There are different DSSs that can support clinicians before, after and even during the procedure. The decisions suggested by the system occur from an organization’s electronic medical record, theoretical importance, and clinician judgment.
Next to the DSS’s, an important field where ML is currently used is radiology. In the field of radiology, a very common procedure is medical imaging. MRI, CT, x-rays, echoes, etcetera. Us humans have come very far and our radiologists are able to identify lots of diseases by looking at a medical image. Though we have become very advanced as a species, our eyes are not able to look at a picture pixel by pixel. Luckily we were smart enough to create something that can: computers. By using ML, the computer can classify the images and predict diagnoses. This makes the diagnosing process for the doctor a lot easier and faster.
When using a CT-scan, radiation is used to visualize the image. As radiation is toxic for humans, this is a harmful procedure and using less radiation would be preferred. This does lead to lower quality pictures, which makes it more difficult for radiologists to draw a conclusion. Luckily, this is not a problem for ML algorithms. Using AI in radiology could thus lead to more accurate results and less harmful procedures.
Natural Language Processing
In almost all hospitals an electronic health record (EHR) is used. Every patient has their own EHR with all its personal and medical data. These EHRs are often complicated and not understandable for a computer. This is where NLP comes in. NLP is a theory-motivated range of computational techniques for the automatic analysis and representation of human language. By using NLP in combination with ML, the EHRs can be comprehended by the computer.
Juhn and Liu performed a systematic review to find out for which diagnoses NLP is most commonly used. They found out that NLP is often used with asthma, atopic dermatitis and allergies. They all use the EHR, and scan it to see if the various requirements to establish the disease are met. If that is the case, the disease is predicted and the caretaker can act accordingly.
NLP can also be helpful in the cardiology department. A study by Ambrosy et al. examined the disease worsening heart failure. This showed that the NLP algorithm could find twice as many patients than were found before. As described above, the algorithm was given several requirements that the patient had to meet. If this was the case, the patient was at risk of worsening heart failure.
This process of NLP has been researched in lots of medical fields and has proven to work. Other examples where NLP was used this way and could successfully predict disorders are: COVID-19, psychotherapy and lung cancer.
Robots
Another application of AI that is used in healthcare are robots. Robots make use of NLP, thus they also use ML.
Robots are currently mostly used for the elderly. They assist the user mentally as well as physically. The robots help the users mentally by reminding and motivating them, but also giving them emotional support. Physically they can hand the user things, deliver items or help them with eating. These robots that help their users at home, are called care robots. Another type of robot is the hospital robot. These robots, in contrast to the care robots, are used in and around the hospital. The main task of hospital robots is handing doctors and nurses supplies, which gives them more time to make contact with patients. The hospital robots that are currently in use only perform non-critical tasks. Another type of robot is the assistive robot. These robots help people that have a disability, such as paralysis. Similarly to the care robots used for the elderly, the robot supports the user with daily tasks that are difficult for the user.
Possible improvements
Although the above developments give the idea that healthcare is already very innovative, this isn’t the case. All of the innovations that are named are only in use in some institutions. This means that these innovations only improve a very small part of care. Thus, the first point of improvement is that healthcare institutions around the world could implement the innovations that already exist. An obvious explanation for why this doesn’t happen as much as it could, is the cost. While this makes sense, healthcare providers should realize that AI innovations save a lot of money and time in the long run as is described earlier on. Per field in AI (ML, NLP and robots) there are still lots of possible improvements.
Machine Learning
As described in the previous section, DSSs seem pretty developed in the medical field. Yet, DSSs have not been developed for every department. In a systematic review by Safdar et al. the use of DSSs for the diagnosis of heart diseases is being evaluated. They found out that though a lot of research has been done and DSSs have been developed, the DSSs are not yet ready to be implemented in hospitals. In an article by Walsh et al. the possibilities of DSSs are researched with the focus on oncology. They describe that a lot has to be done before DSSs can be implemented everywhere. One important step is that the trust of stakeholders, such as clinicians, medical directors, medical insurers and patient advocacy groups, has to be gained regarding the systems. Another important step is the understandance of stakeholders. In conclusion; they have to be taught how the systems work and trust the systems and their outcomes, otherwise the probability of them using it will be low.
In the previous section a DSS in neurosurgery is discussed. Though the system is already implemented, the researchers do notice that it isn’t working optimal and has a lot of room for improvement. This probably is the case with several DSSs.
In short, DSSs are not yet in use in several areas of healthcare, and those that are can be improved. DSSs have proven to improve patient safety, adherence to protocols, reduce costs and help with diagnostics.
Natural Language Processing
Also, NLP has room for improvement. In an article by Zhou and Hripcsak it is explained why and how temporal reasoning is still a challenge regarding NLP with medical data. The definition of temporal reasoning in AI of Cambridge University is: AI research in temporal reasoning focuses on designing automated solutions to complex problems in computation involving time. This is a difficult aspect when it comes to NLP, yet a very important one in the medical field.
Another possible improvement regarding NLP is not only using the data from within the hospital, but all the data that can be gathered from outside and improving the public health with it. In a study of Coppersmith et al, social media is used to prevent suicide. They collected data by reviewing the social media of individuals who were known to have committed suicide. With this data, they were able to identify social media accounts which showed similarities to the social media of those who committed suicide. In the future, similar sources of data could be used to improve our public health.
Robots
In an article by Ozturkcan and Merdin-Uygur it is stated that health care should use humanoid robots in the future to tackle multiple challenges, such as demographic changes, demands for increased quality, limited resources, and cost requirements. They do emphasize the goal should involve creating guidelines that ethically explore the potential of humanoid robots for a positive impact on society. We can also look even further in the future. Vatandsoost and Litkouhi ascertained that all medical procedures, from medical imaging to surgery to medication will lie in the arms of robots. They substantiate this with the fact that robots simply make fewer mistakes than we humans do. These two researches show that a lot is yet possible in health care with the help of robots.
While we are aware that it is easier said than done to implement all these developments, we believe that not enough focus is being placed from within the healthcare sector to accelerate this process.
Possible dangers and how to overcome them
All the innovations described above could help healthcare by saving time or by cost reduction. However, some people may argue that there is a long road ahead of us. It is said that there are risks and challenges in applying AI innovations in healthcare.
The data
The first risk lies in the accuracy of the data. An AI is as accurate as the data it is trained on. In other use cases of AI, accuracy might be less important but in healthcare it is crucial. Incorrect data and biases in datasets can lead to health disparities and incorrect diagnoses which eventually can lead to death. AI applications can be trained with the most comprehensive datasets but still encounter scenarios that they have not been trained on. The quality of the datasets on which AI applications in healthcare are trained is critical for the performance of the algorithm and prevention of incorrect diagnoses or predictions. To minimize the probability of this happening the quality of the datasets used needs to be ensured. The quality of datasets can be ensured by regulations and standards. Regulations and standards for the application of AI in healthcare should be strict in regard to the data used. The data used should be thoroughly investigated for possible errors and biases. The development of these regulations and standards should be a community-driven effort which includes the opinions of clinicians, industry professionals, academia and stakeholders. This will lead to regulations that satisfy everybody and are strict and usable.
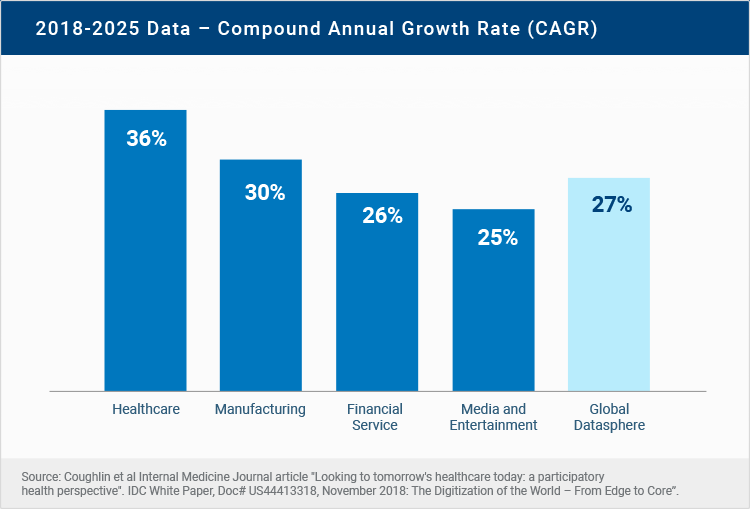
To develop qualitative datasets that are inclusive but without biases and errors seems like a difficult task. However, in healthcare the amount of data created is enormous. RBC reported in 2017 that 30% of the world’s data volume is being generated by the healthcare industry. And is the clear leader in data creation in comparison to other industries, and this means that there is enough data quantity to create a qualitative dataset for the use of AI in healthcare.
Explainability
Other concerns of the use of AI in healthcare mainly address the explainability of AI in healthcare. Explainability is defined as a characteristic of an AI-driven system allowing a person to reconstruct why an AI came up with the predictions. When data is fed to an AI, this AI learns and produces correct predictions. However, the ‘thinking process’ of how this AI came to this answer is often not clear to the people using the AI or even to the people who made this AI. When mistakes are made it is not clear how and why. This is especially crucial in the healthcare domain where mistakes made can lead to harm. Explainability of AI is also a big factor for the application of AI in healthcare. Because if you don’t know how something works, how can you trust it enough to use it?
This is actually a big question in the world of AI and is often called eXplainable AI (XAI) and many people have thought of ways to solve it. As described by Markus et al. There are certainly methods to create an AI which can explain the choices they made. These methods can be divided in to two categories. First of all, the algorithm used for AI can be constructed so that the inner workings of this algorithm are available to the user and it is intrinsically interpretable. However, this will lead to less accurate outcomes and overall decreasing performance of the algorithm. Another option to tackle explainability in AI is the post-hoc explanation. Here the AI used is a complex uninterpretable black box algorithm with accurate results. Explainability is done by reverse engineering the reasoning process of the AI without knowing the inner workings of the AI. These explanation methods can raise trust in the use of AI in healthcare and take away concerns.
In this essay we first gave a global overview of AI innovations that are currently implemented in hospitals somewhere in the world. This led to our most important improvement: sharing data with each other and learning from each other. Next to that, a couple of inventions were named that are not yet implemented but could and should be. Furthermore, there are several concerns with the use of AI in healthcare that might slow down the implementation of these techniques. But these concerns can be taken away with new techniques such as explainable AI and qualitative training datasets.
Because of our big scope we weren’t able to identify every implemented innovation, possible improvement or great dangers. Though we hope to have shown that even though there are some implemented innovations, a lot is possible and a lot of change needs to be made, since the possibilities are there and they could save lives.